Thanksgiving is coming a little later this year, and so are
my blogs on the promised topic of Women’s Health Month. As the weather gets
colder and most high schools are starting their basketball seasons around this
time of year, I thought a great blog topic would be ACL injury with particular
attention to why this injury has a female-athlete predominance.
In 1972, 1 in 27 Varsity sport athletes were female. In
1997, this number drastically increased to about 45%: 55% female: male
participation, thanks to Title IX. With this increase, the number of ACL injuries
also increased with a notable female predominance to ACL injury. This sex
discrepancy in ACL injury begins at puberty and continues into adulthood. Even
more so, the number of non-contact ACL injuries is higher in girls than boys,
and this is a notable increase in incidence that is also seen from the onset of
puberty, age 12 to 14 years in girls. The peak incidence for ACL tear is in the
group of 16 to 18 year-old girls, and the highest numbers of ACL injury have
shown to be in girls’ soccer: 14 per 100,000 female soccer players vs. 4 per
100,000 male soccer players at the high school level. The second highest
incidence is in basketball with the ratio of female: male ACL injuries in this
group of high school athletes being 2:1.
So what’s the deal? Why are ACL injuries more common in
female athletes? To begin to answer this question, we first have to discuss the
biomechanics involved and this boils down to what is an ACL and what does it
do…
What is the ACL
and what does it do?
 The ACL is the anterior cruciate ligament of the knee joint,
and it runs from deep within the distal femur (the long bone of the thigh that
is above the knee) to the front of the tibia (the bigger bone that makes up the
shin). The origin or beginning of the ACL is within the notch of the distal
femur and the proximal (beginning) fibers of the ACL fan out along the medial
wall of the lateral femoral condyle. The ACL attaches to the
tibia on the intercondyloid eminence that is adjacent to the medial meniscus.
All of these interactions allow the ACL, along with the PCL (the posterior
cruciate ligament) to stabilize the knee joint.
The ACL is the anterior cruciate ligament of the knee joint,
and it runs from deep within the distal femur (the long bone of the thigh that
is above the knee) to the front of the tibia (the bigger bone that makes up the
shin). The origin or beginning of the ACL is within the notch of the distal
femur and the proximal (beginning) fibers of the ACL fan out along the medial
wall of the lateral femoral condyle. The ACL attaches to the
tibia on the intercondyloid eminence that is adjacent to the medial meniscus.
All of these interactions allow the ACL, along with the PCL (the posterior
cruciate ligament) to stabilize the knee joint.
Terrible Triad
Because of the interaction of the surrounding stabilizing
structures of the knee joint, a common injury that can occur is called the
“Terrible Triad.” You might hear someone say with reference to this injury that
they “blew out” their knee. This occurs when there is a tear of the ACL, the
MCL (medial cruciate ligament), and the medial meniscus.
So what’s with the
ladies?
There are many theories about why ACL injuries are more
common in the female athlete. The answers have ranged from differences in
female vs. male training, issues with flexibility and ligament laxity,
hamstring/quad strength discrepancy, bone structure, and even female hormones.
So let’s analyze the data and separate fact from fiction, folks.
Hormones
Like everything that affects women, they’ve
tried to blame the female athlete ACL injury predominance on our hormones,
ladies, and guess what? The studies are still inconclusive. The most convincing
theory is that estrogen receptors on ligaments cause increase ligament laxity
in female athletes causing increased risk of ACL tear as opposed to male
athletes.
What
supports this theory:
Some studies have found that there are an
increased number of ACL tears around the time of ovulation (in the
pre-ovulatory and ovulatory phase where estrogen levels peak). Moreover, some
studies have shown that oral contraceptive pills have decreased the risk of ACL
tear in female athletes. The theory behind this would be that OCPs prevent
ovulation, maintain steadier hormone levels, and prevent the changes that make
women more susceptible to ACL tear around the time of ovulation. This theory
has been supported by evidence showing that early on in puberty there is not as
much of a female predominance to ACL tear. Folks have postulated that this is
because estrogen does not vary much at this time, i.e. estrogen is not exerting
its effects on the neuromuscular system.
What
goes against this theory:
Men have estrogen too. What? Well, they do.
But they don’t get the increased joint laxity that is often seen in female
athletes. It may be that their receptors respond differently, but the fact is
that in both boys and girls after puberty, peripheral testosterone is converted
to estrogen, so both sexes have this hormone, which could exert effects on the
neuromuscular system. Other studies have also come about to debunk the idea of
an ovulatory association with ACL tear. They have found a greater number of ACL
tears on cycle days 1 and 2 of the menstrual cycle. These days are during the
first part of menstruation or during the early follicular phase of the cycle
when levels of estrogen and progesterone are low. So what gives? Maybe this one
isn’t actually something we can blame on our hormones, ladies.
Athletic
Training and Conditioning
This argument really used to be something
to think about back in the day when women were just getting into competitive
sports, but now look at us! Go ladies! So proud of where we have taken female
sport!!! :) With female athletics taking off and with Title IX giving women the
same resources to trainers, physical therapists, strength and conditioning
coaches, etc. that male athletes have, we really can’t prove with
evidence-based studies that there are specific differences in the type of
training that male and female athletes are doing which predisposes women to ACL
tears. However, it may be more about what we are NOT doing in our training of
female athletes to compensate for the differences in male and female
musculoskeletal structure and biomechanics. This idea has been linked to
hormones in one study showing that changes in knee joint laxity during the
menstrual cycle does affect knee joint loading during movements, which could be
important in ACL injury prevention programs and how we are training our
athletes. This is just one study done in 2009. So, we need more evidence to
come up with better training programs. But up next, what it is about the female
musculoskeletal system that predisposes
to ACL injury?
Musculoskeletal Biomechanics
Female athletes are more quad and leg dominant;
they rely more on ligaments for stability, and they have increased ligament
laxity, especially after puberty. The intercondylar notch of the femur is more
A-shaped in the female femur vs. the male femur. Women also have a wider
pelvis, which increases knee valgus and causes a greater Q angle.
Bone structure
 So what the heck is knee valgus and Q angle? Knee
valgus is when the knee deviates inward (knock-knees). In many female athletes,
when they jump and land, when they do a deep squat, or when they make a cut to
change direction, their feet are externally rotated, and the hip and knee are
not very flexed. This posturing causes an increase in Q angle, the angle
between the pelvis and the knee. The male Q angle is typically about 14
degrees. The normal female Q angle is about 17 degrees. In persons with
patellofemoral pain syndrome (something we can talk about another time), that
angle is increased to greater than 22 degrees.
So what the heck is knee valgus and Q angle? Knee
valgus is when the knee deviates inward (knock-knees). In many female athletes,
when they jump and land, when they do a deep squat, or when they make a cut to
change direction, their feet are externally rotated, and the hip and knee are
not very flexed. This posturing causes an increase in Q angle, the angle
between the pelvis and the knee. The male Q angle is typically about 14
degrees. The normal female Q angle is about 17 degrees. In persons with
patellofemoral pain syndrome (something we can talk about another time), that
angle is increased to greater than 22 degrees.
Ligaments
The female ACL may also have a lower percent
surface area of collagen.
Muscles
Another consideration is the difference in
strength between genders. By age 15-16 years, girls have 75% of the strength that
boys have, secondary to increase in lean body mass that is much greater in boys.
During puberty, boys increase their hamstring strength by 179% and their quad
strength by 148%. On the other hand, girls become more quad dominant than boys
do with these changes in strength during puberty.
Moreover, when women
experience stress on their ACL, they naturally compensate by activating their
quads and lateral hamstrings, which causes increased Q angle. Yikes!
Immediate
Assessment: Does my child need an MRI?
So we all know that this is my favorite question for
athletes and for all pediatric issues. Parents always want to know if their
children need cat scans, x-rays, and MRIs. With any injury, it is important to
get an assessment from a doctor as close to the injury as possible. Often this
does mean going to an Urgent Care Center or Emergency Room as most sporting
events take place after regular pediatric or orthopedic office hours. The
opportune time for assessment of ACL tear is actually immediately after the
injury occurs, so if your team has a Sports Medicine doctor available at the
game, this is your best bet. Even waiting until you get to the ER after the
game can sometimes make assessing an ACL tear more difficult because the more
swelling that occurs, the more difficult it is on physical exam to evaluate the
ACL.
The most important thing is to be evaluated shortly after the injury has
occurred. You will not be able to get an emergent MRI, and an MRI is
not always necessary in the case of knee injury. Depending on the mechanism of
injury and the physical exam, your doctor may think an x-ray is necessary to
rule-out fracture. The next step may be an MRI to evaluate ligaments and other
soft-tissue damage, depending on the physical exam. Your child does not need a
CT or cat-scan. This test is emergently available, but it is not as definitive
as MRI and has, as we have previously discussed, a large amount of radiation,
and should not be done unless absolutely necessary. Listen to your doctor and
ask questions if you do not understand the tests ordered or the plan for the
care of your child.
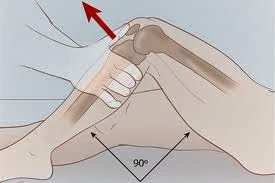 |
| Anterior Drawer Test - one of the physical exam tests to evaluate for ACL tear. |
Treatment
Interestingly enough, these days, for an ACL tear, depending
on the severity, and depending on the future goals of the athlete, you do not
always need surgery! Isn’t that great news? It depends on how severe the tear
is and how competitive and lengthy the athlete’s future career will be. It is
often helpful to get the opinion of two different orthopedic surgeons before
making your decision on surgery. This injury used to be a career-ending injury
for many athletes, and now recovery times and strong commitments to rehab have
athletes back to jogging in 6 weeks and back to their sport within the same
season, depending on when the injury occurs.
Prevention
I hope that what this short article has shown you is that we
actually need more studies to show what we should be doing to protect our
athletes, what strength and conditioning programs would best help prevent ACL
tear. Studies have shown that the types of prevention programs that are in the
mix currently have made no difference for kids age 9-12 years in preventing ACL
tear; however, they have noted improved technique and better prevention with
programs in the age range of 14- to 17-year-olds. These kids may be more
susceptible to feedback and coaching at this age, but 9- to 12-year-olds are
kids already learning sport-specific skills, and we need to find a program that
can work for improving their techniques in order to prevent ACL tear and other injuries.
One thing is for sure, our treatments and our rehab have come a long way in
helping athletes recover from these injuries, but prevention is definitely the
future for our athletes.
References:
Bell DR, et al.
The effect of menstrual-cycle phase on hamstring extensibility and muscle
stiffness. J Sport Rehabil. 2009
Nov;18(4):553-63.
Bell
DR, et al. The effects of oral contraceptive use on muscle stiffness across the
menstrual cycle. Clin J Sport Med. 2011
Nov;21(6):467-73.
Dragoo JL,
Castillo TN, et al. Serum Relaxin Concentrations and ACL Tears. Journal of
Sports Medicine. 2011. 39:2175-2180.
Lefevre N, et al. Anterior cruciate ligament tear during the menstrual
cycle in female recreational skiers. Orthop Traumatol Surg Res. 2013 Sep;99(5):571-5.
Park SK, et al. Alterations in knee joint laxity during the menstrual
cycle in healthy women leads to increases in joint loads during selected
athletic movements. Am J Sports Med. Jun;37(6):1169-77.
Slauterbeck, et al. The Menstrual Cycle, Sex Hormones, and Anterior
Cruciate Ligament Injury. Journal of Athletic Training 2002;37(3):275–280.
Wild CY, Steele JR, Munro BJ. Why do girls sustain more anterior
cruciate ligament injuries than boys?: a review of the changes in estrogen and
musculoskeletal structure and function in puberty. Sports Med.
2012 Sep 1;42(9):733-49.





No comments:
Post a Comment